
Measuring malnutrition
The low cost hand-held device was designed and developed by a University of Sydney research team to measure the early stages of infant malnutrition.
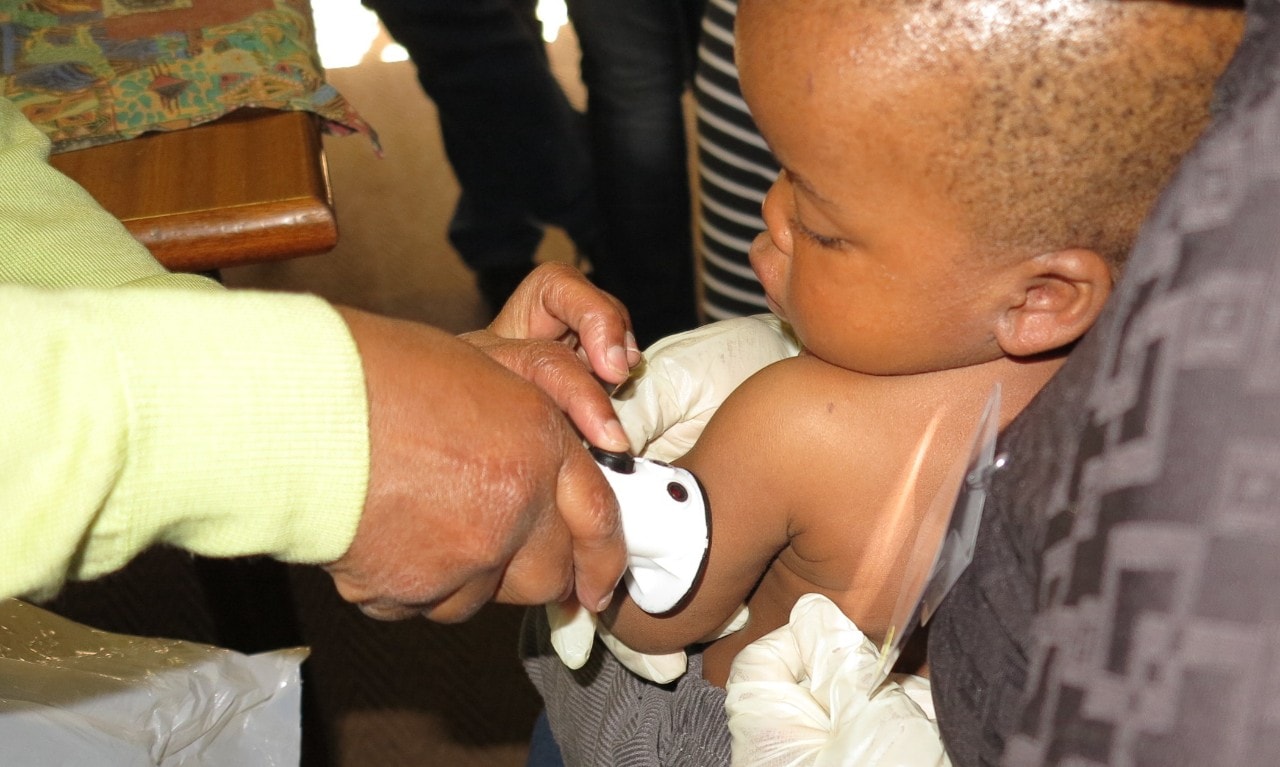
Researchers has conducted successful trials of the NIR device in clinics in Soweto, Africa
A team jointly led by Dr Alistair McEwan, an electrical and information technologies engineer at the University, and honorary Professor Heather Jeffery, a specialist in maternal and child health, are conducting successful trials of the device in Soweto, Africa.
NIR is a highly accurate technology that uses multiple wavelengths to separate a human’s body components such as temperature, melanin, water, dermis, muscle or fat under the skin
Designs of the revolutionary malnutrition screening device have been published in the journal Scientific Reports.
The unit developed by the team uses near infrared (NIR) to assess an infant’s body composition and is suitable for use in areas where there is limited electricity supply and technical expertise.
Dr McEwan says: “The portable and easy-to-use device uses light to measure the amount of fat under the skin so that infants don't need to be placed in a scanner or have a skin pinch test.
The device can be made inexpensively with only five sensors and the length or height of the infant does not need to be measured, avoiding a difficult measurement of infants who wriggle and protest at being held flat.
“Light in the NIR range is used where our skin is transparent; this type of light is not visible to humans for example on a TV remote control, but can be sensed by nocturnal animals and snakes.”
Dr McEwan explains: “NIR is a highly accurate technology that uses multiple wavelengths to separate a human’s body components such as temperature, melanin, water, dermis, muscle or fat under the skin.”
“The human skin is transparent in NIR light over a certain range of wavelengths. Our studies have shown that fat absorbs NIR and fat levels can be determined at five wavelengths.
Professor Heather Jeffery says: “Low fat composition in newborns exposes them to an immediate risk of increased mortality and morbidity, and to diabetes and obesity diseases in later life.”
“The lack of convenient, low-cost devices for monitoring nutrition has led to difficulties for health workers trying to identify malnourished infants, and in monitoring changes in the nutritional status of an infant who has received interventions,” she says.
The team that also included early career researchers Dr Angela Carberry, Dr Peter Jones and PhD candidates Jacqueline Huvanandana and Fatin Hamimi Mustafa, are working alongside the University of Oxford’s INTERBIO-21st study to test their prototype device for suitability in different skin tones and in large communities in Africa.
Dr McEwan oversees the University of Sydney's bioelectronics program, combining electrical engineering and biology to make inexpensive physiological monitors that reduce the strain on public health budgets.
The team’s work was support by Phase II funding through Grand Challenges Explorations, an initiative created by the Bill & Melinda Gates Foundation that enables individuals worldwide to test bold ideas to address persistent health and development challenges.
Related articles
Psylo partnership to deliver psychedelic treatments for mental health
