Uncovering the mystery of migraine
It's a disease that has baffled health professionals for years, but our researchers have taken a significant step forward in understanding migraine.
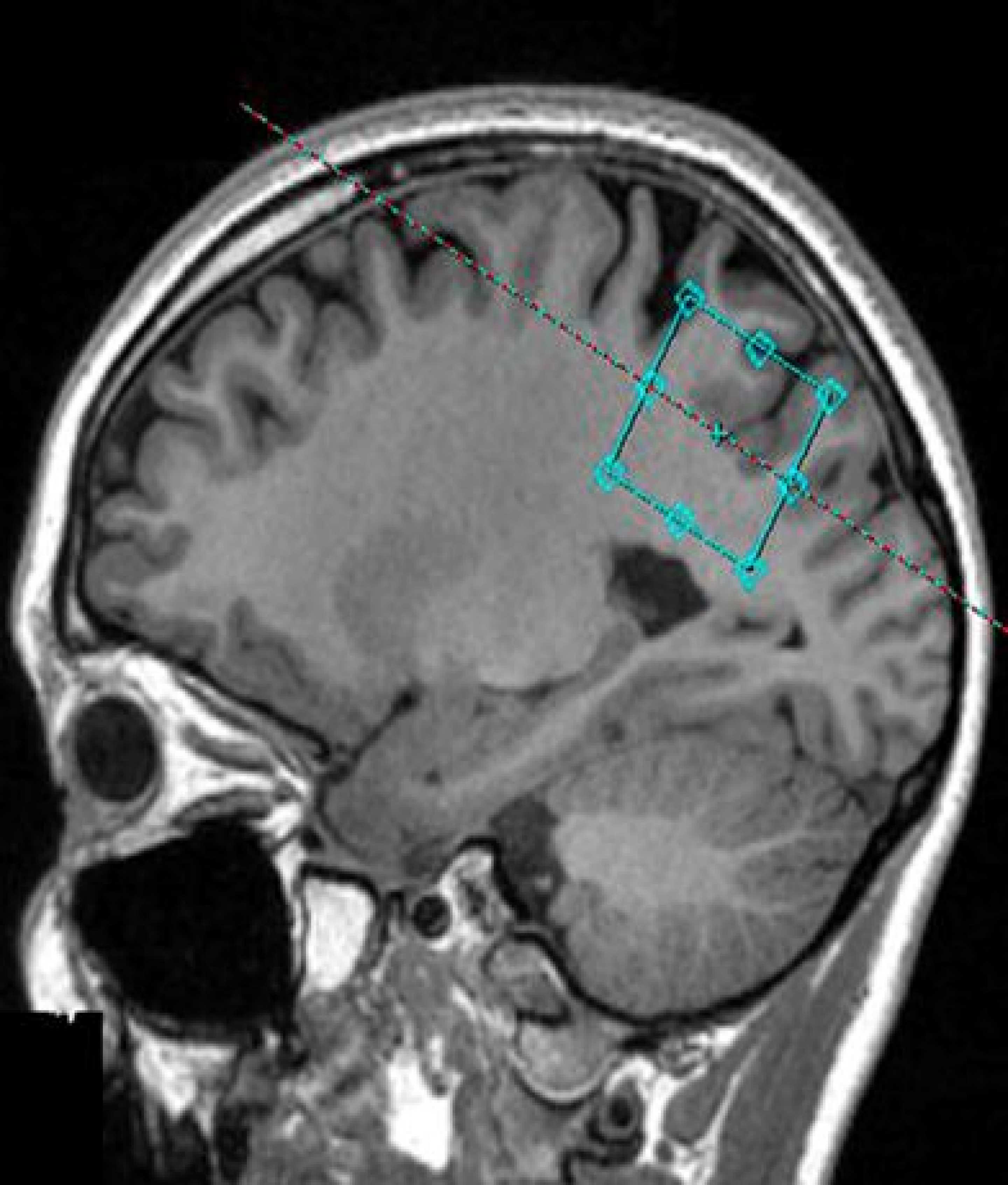
MRI brain scan indicating area of the brain where GABA is measured
A new study, published in NMR in Biomedicine, reveals higher levels of the chemical gamma-aminobutyric acid in the brain of migraine sufferers, supporting the theory that migraines are linked to a chemical imbalance in the brain.
"The finding paves the way for the discovery of new, effective treatments for migraines," said lead researcher Maria Aguila, PhD candidate in the Faculty of Health Sciences.
"For such a debilitating condition, very little is known about migraine so this is a big step forward and could lead to better diagnosis and treatment of the disease in the future," she said.
Gamma-aminobutyric acid or GABA as it is commonly known, is the most abundant inhibitory brain chemical and has long been suspected to play a role in migraines due to its ability to influence pain. This study is the first to accurately measure GABA levels in the living brain.
"We still don't know what causes migraine, how it starts and ends, or why the triggers appear to differ from one person to the next, but this discovery means that we can now be much more specific with our research going forward," said Ms Aguila.
"For example, GABA could be used to help us identify migraine sufferers and track responses to drug trials, and measuring GABA levels over a period of time could well reveal what’s causing attacks.”
The study compared the levels of GABA in twenty chronic migraine sufferers to an age and gender matched control group who did not experience any form of regular headaches. Brain scans were conducted when the participants were not having a migraine.
The measurement of GABA levels in the brain was made possible by a novel spectroscopy technique associated with MRI developed by researchers at the University of Sydney Brain and Mind Centre.
Associate Professor in Neuroimaging, Jim Lagopoulos said the ability to directly measure these chemicals in the brain would not have been possible several years ago.
“These advances not only allow us to study fundamental changes in brain chemistry that are associated with migraine, but they also open a whole new world with respect to monitoring a patient's response to treatment and compliance," he said.
The researchers were unable to tell if the increase in GABA is related to a recent migraine attack or signalling a new one as the scanning process is currently too complex to carry out during a migraine attack.
The study design was conceived by Professor Kathryn Refshauge and executed by researchers from the University of Sydney’s Faculty of Health Sciences and Brain and Mind Centre, Neuroscience Research Australia, University of the Philippines and University of New South Wales.
Related articles
Surge in flu this winter
People suffering severe flu this winter should seek medical treatment as soon as possible.

Dementia tsunami: Alzheimer's and other dementias to triple by 2050
Governments need to take action on delaying the onset of Alzheimer's disease and other dementias, argues Associate Professor Lesley Russell.
Ready, set, Rio: Sydney cohort heads to the Games
As more than 3.5 billion people around the world turn their sights towards Rio this week, 30 athletes from our community are getting ready to take their place on the globe’s biggest sporting stage.
Australian study wants your view on personal genomic testing
Do you want to know about your genetic information? Would you share it?
Maternity care for Aboriginal women
A new maternity services plan for Aboriginal and Torres Strait Islander women in rural and remote communities is urgently required, a report has found.
World-beaters join Brain and Mind Centre to defeat dementia
Three world-leading neuroscience scholars are joining the University of Sydney’s Brain and Mind Centre to progress research-led treatments for dementia and other neuro-degenerative diseases affecting human memory and thinking.
Study explains elastin's remarkable movements
New research likens the flexibility of elastin in a blood vessel to the dynamics of a ballet.
